
20 Jan Is Isotretinoin (Roaccutane) Dangerous?
Acne vulgaris is a very common skin condition that affects 80% of teenagers and adults. From milder forms such as comedones (blackheads and whiteheads), pimples (papules and pustules) to severe types such as cysts and nodules- most of us would have encountered acne in its various forms in our lives.
As I’ve shared in my previous blogpost Acne: Types, Causes, Treatments and Tips for Prevention, acne vulgaris is a complex skin condition. Although the pathogenesis or steps in the formation of pimples are large similar, factors and severity differ from person to person, which in turn affect treatment outcomes.
Acne treatment
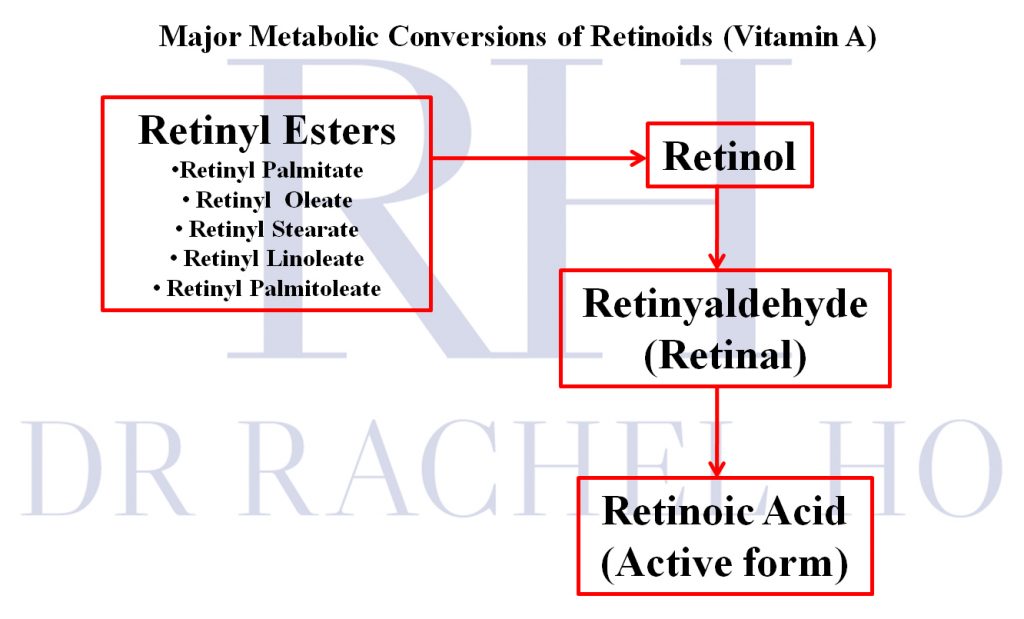
One mainstay of treatment for acne is retinoids. Retinoids are a family of active ingredients that are derived from vitamin A. There are different types of retinoids- retinols, retinaldehydes, retinoic acid…etc. The potency and efficacy of each of them differ. You can read the details about the differences between these retinoids in The Beginner’s Guide to Starting Retinoids.
Related blogpost:
5 Affordable & Popular Retinoids Reviewed
Skinbetter Science’s Alpharet Overnight Night Cream
My previous blogposts have looked at topical retinoids (including retinoic acid). This blogpost will focus on oral iostretinoin, which is also known by its trade names Nimegen, Roaccutane, Oratane…etc. In my years of treating patients with acne, one mention of Roaccutane or Nimegen is usually met with fear of warnings of side effects from my patients. This review will help you to understand some of the safety issues, side effects and myths about isotretinoin. I hope that this educational poste will give you a better understanding of isotretinoin and acne treatments.
How does Isotretinoin work?
Oral isotretinoin contains retinoic acid. It is also known by its brand names such as Nimegen, Roaccutane, Accutane, Oratane…etc. Isotretinoin received US FDA approval for the treatment of severe acne 1982. In more recent decades, isotretinoin has also been used to treat milder forms of acne that are not improving with other forms of treatments.
Isotretinoin combats acne by vulgaris by targeting all four steps in the pathogenesis of pimples. Use of isotretinoin has been found to:
• Reduce sebum production
• Lower C. acnes count
• Decrease comedone formation
• Reduce inflammation
To date, isotretinoin is the only drug that impacts on all four major factors implicated in acne vulgaris. Compared to its topical equivalent, retinoic acid (rectanyl or Stieva-A); Isotretinoin has greater sebum reducing effects. Isotretinoin is also considered the most effective medication for treatment of acne vulgaris. There are no other medications that have superceded the efficacy of isotretinoin to date. However, isotretinoin is not liberally prescribed as this drug because of its potential side effects and adverse drug reactions.
Isotretinoin: Why Is This Medication So Feared?
Birth defects in pregnant women
The top concern about isotretinoin among my female patients especially is the risk of birth defects; which is valid. Isotretinoin is a known teratogen and has a high risk of birth defects when used during pregnancy. The history of Accutane prescription in the US has been marked by birth defects and public backlash. After Accutane was made available in the US, reports of birth defects in women who consumed Accutane during their pregnancies started to surface. The birth defects in babies include craniofacial, cardiovascular, neurological and thymic malformations. The risk of babies being born with these malformations from Accutane use during pregnancy is estimated to be 20-35%. Even for children who were born looking normal after their mother consumed Accutane during pregnancy, the risk of neurocognitive delays is 30-60%.
Isotretinoin is considered to be a US FDA Pregnancy Category X drug. It should not be used in pregnancy at all. You can read more about pregnancy safe and un-safe skincare in Pregnancy Skincare Guide: What’s Safe and What to Avoid.
Association with depression
Case reports have linked depression with isotretinoin use. However, clinical trials have been more reassuring- with larger studies showing that isotretinoin use did not encourage negative mood or depression. Acne is also associated with depression, so the association between isotretinoin and depression may be incidental.
What are the side effects of Isotretinoin?
The most common side effects of using isotretinoin are related to the skin. Dryness of the skin, lips and mouth are fairly common; so remember to moisturise and use ingredients that repair the skin barrier. If you wear contact lenses, you may also experience dry eyes. Some patients may experience skin peeling and flaking as well as rashes.
Related blogposts:
Ceramides in Skincare: A Relief for Dry & Sensitive Skin
Everything You Need to Know About Hyaluronic Acid
5 Cult Favourite Hyaluronic Acid Serums and Moisturisers Reviewed
Increased sun sensitivity also occurs with Isotretinoin use. With unprotected sun exposure, you have an increased risk of sun damage to the skin. Sunburns, hyperpigmentation, fine lines and dull skin are examples of sun damage. Sunscreen use is encouraged; choose n oil-free and non-comedogenic sunscreen for acne skin.
Related blogposts:
Hyperpigmentation Disorders: Types, Causes & Treatment
How to Lighten Pigmentation and Dark Spots with Skincare
Sunscreen Reviews: the Best, the Worst and Unsafe Ones
Sunscreen Beyond the Basics: Controversies, Trends & FAQs
Less common side effects of isotretinoin are muscle and joint aches; headaches and gum inflammation. Isotretinoin has also been linked to raised cholesterol and triglyceride levels in the blood and as well as raised liver enzymes. Liver function derangement due to isotretinoin use is very uncommonly and mostly mild and asymptomatic.
As discussed above, the risk of fetal abnormalities if taken during pregnancy cannot be overemphasised.
ACCTUANE NOSE JOB?
Recently on TikTok, some users have shared that Accutane or Isotretinon has made their noses look slimmer and smaller; and referred to this effect as “Accutane nose job”. Why is this so? Accutane or isotretinoin also has the effect of reducing the size of the sebaceous glands. The nose has a high density of these oil glands; and accutane/ isotretinoin could theoretically cause the nose to look slimmer and smaller as a result of shrinking the oil glands. However, the results of this “accutane nose job” is very minimal and the effects are temporary. To get more significant augmentation of your nose, consider rhinoplasty or non-surgical alternatives such as nose fillers or nose threadlift. Isotretinoin alone will not change the structural anatomy of the nose like the cartilage and bones.
What must I know before starting Isotretinoin?
Prior to starting isotretinoin, your doctor will perform a blood test to assess your liver function and cholesterol and triglyceride levels in your blood.
For female patients with acne, there is a strict protocol to ensure that you are not pregnant or do not become pregnant while using Isotretinoin. Prior to stating isotretinoin, a pregnancy test (urine or blood) will be conducted. If you are expecting, you cannot be started on isotretinoin. Use of birth control methods and contraceptives are necessary when you are taking this medication. If you wish to conceive, isotretinoin has to be stopped for at least one month and you have to use contraceptive methods during this period too.
Blood donation is also not advised while you are on isotretinoin. This is to prevent blood containing this medication from being given to a pregnant female.
Retinoic acid cream is one alternative to isotretinoin
What are the alternatives to Isotretinoin?
There are alternatives to using isotretinoin for treating acne vulgaris. Topical retinoids and oral medications like antibiotics and hormonal therapies are some examples of therapies for acne vulgaris. However, each of these medications targets different pathways in the pathogenesis of pimples and have different efficacies. You can read more about more topical retinoids and how they work in The Beginner’s Guide to Starting Retinoids. Adjuvant medical treatments like chemical peels, Q-switched lasers and LED therapy are also effective in improving acne. I use a combination of these in my clinic in Singapore- the faster the pimples are cleared, the lower the likelihood of post inflammatory hyperpigmentation and acne scars.
Related blogposts:
10 Things to Know Before Having Lasers for Your Pigmentation
The Truth About Chemical Peels
Severe acne and nodulocystic acne are the main indications for starting isotretinoin. Nodules and cysts also benefit from cortisone/ steroid injections to prevent scarring. You can read about intralesional steroid injections for cystic acne in Acne Steroid Injections & When Popping A Pimple Could Kill You.
I hope that this blogpost sheds more light on isotretinoin. It is a powerful medication for treating severe acne and acne that is not responding to treatments. Although there are side effects associated with consuming Accutane, precautionary measures for patients (especially female patients) can help to reduce the risk of adverse events. You can read more about acne and pimples in these posts:
Acne: Types, Causes, Treatments and Tips for Prevention
Maskne: How to Avoid Acne from Wearing Face Masks
Acne and Diet: Foods to Avoid for Less Pimples
Fungal Acne is Not Acne at All: Malassezia Folliculitis Explained
How to Get Rid of Large Pores: Myths and Truths









No Comments